
The Global Polio Eradication Initiative (GPEI)
The initiative
The World Health Assembly (WHA), the annual meeting of the Ministers of Health of all WHO member states, first committed itself to polio eradication in 1988. The assembly called for the worldwide eradication of the disease by 2000. It marked the launch of the Global Polio Eradication Initiative (GPEI), which was spearheaded jointly by national governments, the WHO, Rotary International, the US Centers for Disease Control and Prevention (CDC), and UNICEF.
Although significant progress had been made as a result of the GPEI, in May 2012 the WHA declared the completion of polio eradication a programmatic emergency for global public health. It called for a marked increase in the intensity of eradication activities in the poorest performing regions.
"The Polio Eradication and Endgame Strategic Plan 2013-2018 is a comprehensive, long-term strategy that addresses what is needed to deliver a polio-free world by 2018. This strategic plan is the currently in force and the major objectives of the plan are:
- Detect and interrupt all poliovirus transmission
- Strengthen immunization systems and withdraw oral polio vaccine
- Contain poliovirus and certify interruption of transmission
- Plan polio's legacy.” [1]
“In all three remaining polio-endemic countries (Pakistan, Afghanistan and Nigeria) national Emergency Action Plans were established to overcome the remaining barriers to reaching every child with polio vaccines; in each country, oversight bodies reporting to heads of state were further extended from the national to subnational levels to intensify political and administrative accountability for the quality of key eradication activities.” [2]
The challenge
Polio is a viral disease that can cause paralysis and sometimes death. It has been largely eradicated from the Western world as a result of infancy and childhood inoculation. However, it was for much longer a serious problem in the developing world.
Polio often spreads among dense populations amid poor sanitation, and occurs most frequently in the summer. Children under the age of five are the most vulnerable to polio. In the late 1980s the World Health Organization (WHO) recognised the need for a combined effort to control and eradicate the disease altogether.
The public impact
The initiative has been largely successful. “Since its launch at the WHA in 1988, the GPEI has reduced the global incidence of polio by more than 99%. More than 10 million people are walking today who otherwise would have been paralysed.” [3] It has achieved this by immunising 2.5 billion children since its inception.
There is constant progress towards eradication, but it is not yet complete. “In 2012, India stopped the virus, and in 2015 Nigeria was removed from the list of endemic countries. Polio is found only in Pakistan and Afghanistan, and fewer than 100 cases were reported in 2015.” [4]
Stakeholder engagement
The main stakeholders are the WHO and its member states. The GPEI partners include:
- “The Bill & Melinda Gates Foundation. [5]
- The United Nations Foundation and other private foundations.
- Development banks (e.g., the World Bank).
- Donor governments.
- The European Commission.
- Humanitarian and nongovernmental organisations (e.g., the.
- International Red Cross and Red Crescent societies).
- Corporate partners (e.g., Aventis Pasteur, De Beers).
- Volunteers in developing countries.”
Since the establishment of the GPEI, the stakeholders in the polio eradication drive have been instrumental in achieving near-eradication. This is evident from the fact that the GPEI has been able to raise about USD10 billion up till now to carry out its programme across the world. The 2013-18 Plan was formulated in consultation with its many partners, such as WHO, UNICEF, subject experts, and governments.
Political commitment
In 1988, the 125 WHO member states (there are now 194) made a definitive commitment at the WHA by creating the GPEI. In nearly three decades since then, the WHO and its members have contributed to its continued funding and have, in general, vigorously pursued immunisation programmes in their own countries.
In September 2012, government leaders in the endemic and donor countries and the UN secretary-general declared that eradicating polio was a top priority. This signalled the political commitment needed to effectively implement national the Emergency Action Plans and achieve the desired endgame.
Public confidence
The success of the GPEI indicates high levels of uptake in the vaccine implying good public confidence. However, the initiative has not been without hiccup. For example in the predominantly Muslim Uttar Pradesh community in India and Northern Nigeria, rumours that the oral polio vaccine caused sterility resulted in a vaccine boycott. The authorities were aware that lack of confidence could hinder the campaign, so took preventative action by building a community of ‘social mobilisers’ in high risk communities. [6]Clarity of objectives
The GPEI's objectives are clear: eradicate polio from all the nations of the world. As more nations, such as India and Nigeria, are declared polio-free, the GPEI's sights are trained more narrowly on those countries that still have the disease: Pakistan and Afghanistan.
All 194 WHO member states are currently engaged in establishing that, by 2018, all regions of the world will be polio-free and ensuring that all poliovirus stocks are safely contained.
Strength of evidence
The GPEI has always based its programmes on sound medical evidence, and over its life has built up its own knowledge and experience in immunising children against the virus. For example, the 2013-18 Plan “is based on the epidemiology of polio globally at the end of 2012, the recent rate of oral polio vaccine (OPV) campaign quality improvements in the remaining polio-infected areas, new understanding of the risks posed by vaccine-related polioviruses, and the recent development of new strategies and tools for managing post-eradication risks”. [7]Feasibility
The high levels of funding and the active involvement of WHO member states and NGOs has meant that the GPEI's goals were always achievable. This is as true of the endgame as of the initial strategy:
"A thorough activity and cost analysis was conducted by the GPEI, resulting in a budget of US$ 5.5 billion to achieve the [2013-18] Plan's objectives through 2018 ... The budget includes the cost of reaching and vaccinating more than 250 million children multiple times every year, monitoring and surveillance in more than 70 countries, and securing the infrastructure that can benefit other health and development programmes.” [8]
Management
The GPEI is a well-structured and well-run organisation:
- “The WHA issues the resolutions that determine the scope and direction for the GPEI. [9]
- “The Initiative operates within a broad framework of intergovernmental and interagency cooperation and participation.
- “The Polio Oversight Board (POB) oversees the management and implementation of the GPEI through its core partner agencies. The POB is composed of the heads of GPEI core partner agencies, who meet quarterly to review GPEI operations and ensure high-level accountability across the GPEI partnership.”
- “The POB's decisions are executed through the Polio Steering Committee (PSC) and its core subsidiary bodies. [10]
- “The Polio Partners Group (PPG) informs the work of the POB, represents GPEI stakeholders and donors and ensures the GPEI has the necessary political commitment and financial resources to reach the goal of polio eradication.
- "National authorities have primary responsibility at all levels of government for the achievement of the Plan's objectives.”
Measurement
There is an Independent Monitoring Board whose role [is to “independently evaluate progress towards each of the major milestones of the GPEI”. [11] For example, in the 2013-18 Plan, “A Monitoring Framework will be used to assess progress against the four objectives and corresponding milestones laid out in the Plan.” [12]
This involves regular and relatively frequent reviews. “A mid-term review was conducted for the plan in mid-2015 ... The review concluded that while the strategic plan remains a strong framework for ending polio, there is an urgent need to re-focus certain priorities and activities. This includes strengthening surveillance, improving the quality of immunization campaigns and building capacity to respond to outbreaks. Based on these recommendations, the review also evaluated the deadline for eradication, and any resulting financial implications.”
Alignment
There is a strong alignment of interest among stakeholders and partners, led by the WHO, and including the donor NGOs, private organisation and the WHO member states: “national governments in both polio-affected and polio-free countries play a critical role in maintaining sensitive surveillance and high population immunity, including through strengthened routine immunisation services”. [13]
An example of alignment is demonstrated in the way that new approaches to vaccination are adopted. “The Strategic Advisory Group of Experts on immunisation (SAGE) reaffirmed that the globally coordinated switch from trivalent oral poliovirus vaccine to bivalent should occur in April 2016 ... SAGE's landmark decision had previously been endorsed by the WHA in May 2015, when Ministers of Health from 194 member states adopted a historic resolution on the global effort to eradicate polio, paving the way once and for all for a lasting world free of both wild and vaccine-derived polioviruses.” [14]
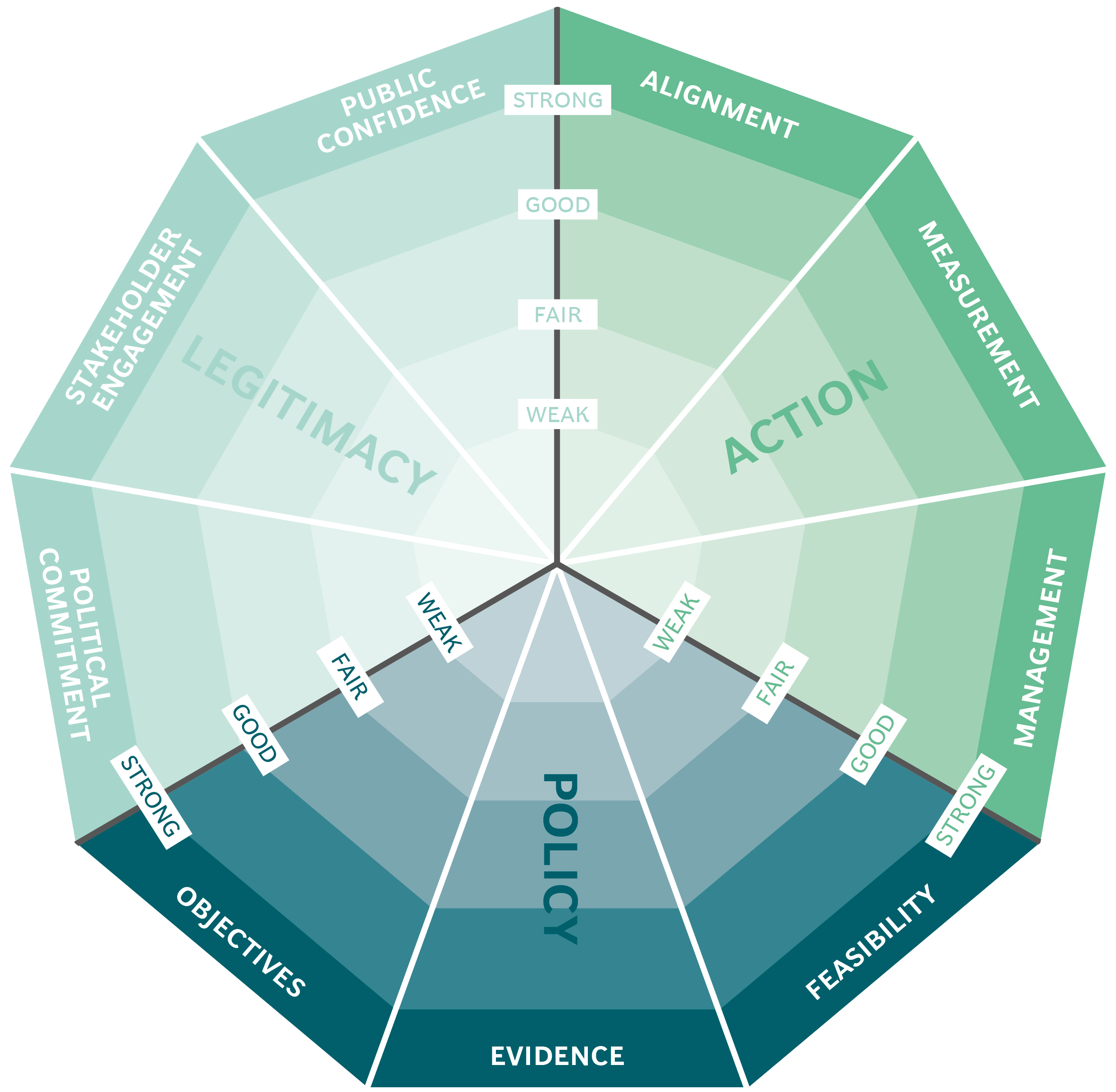
The Public Impact Fundamentals - A framework for successful policy
This case study has been assessed using the Public Impact Fundamentals, a simple framework and practical tool to help you assess your public policies and ensure the three fundamentals - Legitimacy, Policy and Action are embedded in them.
Learn more about the Fundamentals and how you can use them to access your own policies and initiatives.
You may also be interested in...


Organ Donations in Iran

Legislating to encourage organ donation in Israel

GAVI, the vaccine alliance

WHO: delivering insecticide treated nets to control malaria
